There has been an overwhelming deluge of information and some confusion around the use of face masks to limit the spread of coronavirus in recent weeks. I thought I would put my science background (I studied coronaviruses for my PhD) to good use and try to summarise the deluge of new information into something more digestible to the lay-person, in particular those looking to make or buy a handmade face mask.
Please, if you take nothing else from this post, remember this….
Wearing a homemade mask alone will not prevent you from catching Coronavirus, hand-washing and social distancing are still needed but wearing a mask is widely accepted to help keep us from unwittingly spreading the virus.
What masks do most effectively is limit the spread of virus from people who are not yet showing symptoms to other people. While they make it more difficult for you to touch your nose and mouth they will not stop you touching a contaminated handle and then rubbing your eyes. Social distancing (keeping 2 m / 6 feet away from anyone you do not live with), avoiding touching your face while out of your home and scrupulous hand hygiene are still your best bet for avoiding this nasty infection.
Think of mask-wearing as an act of altruism, you are protecting everyone else from the virus that you might be breathing out without even knowing that you have the infection. Between 20 and 50% of people infected with coronavirus do not know they have it and there have been documented instances of asymptomatic carriers infecting other people (Mizumoto, Nishiura). Masks are most effective in limiting viral infections if everyone wears them while in confined public spaces.
Most of the world has now adopted a policy of wearing masks in enclosed public spaces (public transport and shops are key hot spots where you might have close encounters with people you do not live with), it looks like face masks are here to stay.
Please don’t rush out to buy an N95 mask or surgical face mask, our healthcare workers (from doctors to nursing home assistants) need these much more than we do.
Another issue with the general public using disposable, medical-grade face masks is the environmental impact, they contain synthetic materials that will take centuries to degrade, piling up in land-fill sites for generations to come. Unfortunately, washing and reusing them is not an option for most of these masks, they disintegrate and lose their filtering integrity if you put them in the washing machine. Making or buying a reusable face mask is far more eco-friendly and sustainable for the planet.
Which materials make the best face masks?
There have been several papers submitted or published on this topic recently, some with very exciting results but I think we need to consider the data regarding particle size penetration of different materials with a healthy dose of scepticism. These data are generated in a lab with specialist equipment and as such are a useful starting point but do not take into account human behaviour or the “sticky-ness” of virus particles and the liquid droplets they are invariably carried in when a person talks, coughs or sneezes. These studies are conducted by blowing particles of a known size through samples of fabric and then measuring how many particles reach the other side.
This area is a rapidly evolving topic of research, I fully expect mask material recommendations will be updated multiple times in the coming weeks and months.
What do N95 N99, FFP-2 and FFP-3 mean?
These masks are seen as the gold standard and are currently in short supply as they are are single-use items, desperately needed by front-line medical staff.
FFP-2* (Filtering Facepiece against Particles) and N95 meet equivalent standards, the materials of both masks will trap at least 95% of 0.3 micrometer (um) diameter particles.

FFP-3 and N99 are broadly equivalent to each other too, trapping at least 99% of particles.
As with all masks, how well they fit an individual will impact their effectiveness, this is particularly true in children (van der Sande).
While coronaviruses, measuring 0.1-0.2um, are smaller than the 3um particles used to test commercial dust masks and respirators they are expelled from the body (through talking / coughing / sneezing) in fluid droplets, and these droplets are typically 0.1-10um in diameter (Zayas).
*FFP is most commonly used in Europe and sometimes you will see FFP2 / FFP3 abbreviated to P2 / P3.
Breathability
When selecting a mask material there has to be a trade-off between breathability and particle filtration (how many particles will be let through). At its extreme, plastic sheet may give 100% protection against virus particle transmission but it does not allow the wearer to breath so is useless as a mask material. At the other end of the spectrum, cotton scrim has large open holes between the threads, it is very easy to breathe through but also allows even large particles to pass through unhindered.
Recommendations for mask material selection
Up until last week, I was making masks with good quality quilter’s cotton fabric (at least 80 threads per inch), which had been recommended by several research groups, and a layer of flannel (I suspected that the fluffy surface of flannel would capture more particles but had not read any papers that had tested it as a material).
Then, last week I stumbled across a very exciting paper. It was submitted on 24th April to the American Chemistry Society Nano (I know, not looking very exciting so far but bear with me…). This team reported on the effect of combining different materials to improve small particle filtration without sacrificing breathability (Konda). Some of the combinations they tested performed better than the surgical masks and were on a par with the N95 masks under laboratory conditions. This table summarises their most promising materials:
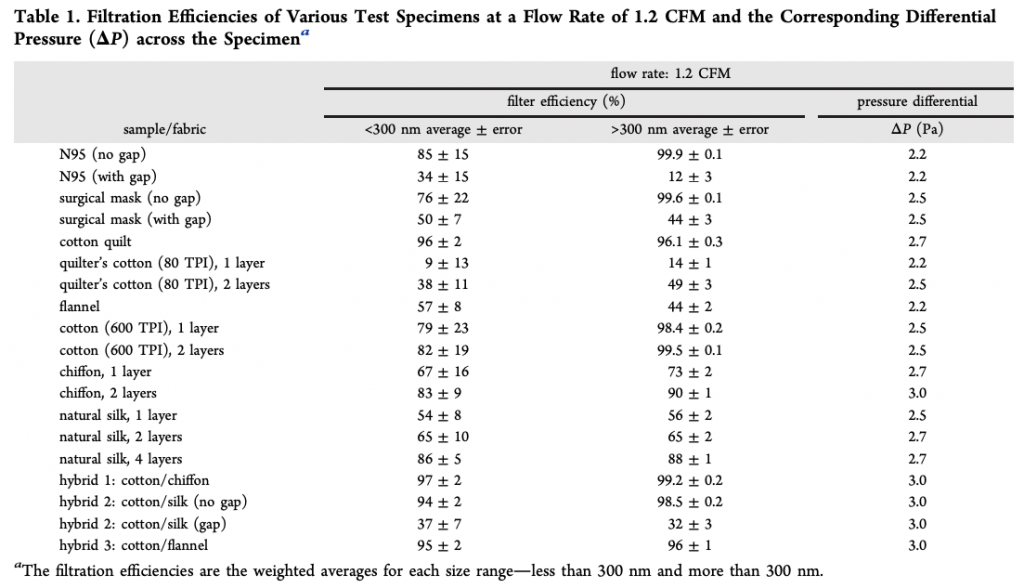
As mask makers, we are most interested in the left hand column, the less than 300 nm column. 300 nm = 0.3 um and if your recall, coronaviruses are roughly 0.1-0.2 um in size, so in aerosol form they will come under that column but in droplet from they would most likely be in the middle column for particle size, however, these larger droplets tend to fall to the ground quickly so you are less likely to be breathing them. The higher the number in these 2 columns the better, this reflects the percentage of particles that the material has trapped.
The column on the right is a reflection of how breathable the fabric combinations are, i.e. how hard you have to breathe to move air through the layers of fabric. Although slightly increased in comparison to the N95 and surgical masks the researches indicated mask wearers would be unlikely to tell the difference in practice.
I was disappointed that the researches did not share which type of “natural silk” they used, they do not appear to be aware that silk fabric is available in a very wide range of weights and unlike some of the other fabrics tested, they did not provide a supplier either. I am going to assume they used a medium weight (5-8 MM) as 4 layers of heavy-weight (12MM) silk would be quite difficult to breathe through.
The results for silk fabric are likely to be of interest if you are thinking of folding a cotton bandana looped over 2 elastic bands to create a makeshift face covering, you might want to reach for a silk scarf instead!
Which shape mask should I make?
The Konda et al group were keen to point out that a poorly fitting mask significantly reduces its ability to filter particles, even the much coveted N95 mask only managed to filter 34% of particles if the mask did not form a tight seal. This seems rather obvious, if there is a gap between your skin and the mask, air is going to take the route of least resistance and flow through the gap rather than the material. Therefore, finding a mask shape that fits snugly is at least as important as choosing the right materials.

Thousands of different face mask designs / templates have been shared online in recent weeks, many with accompanying instructions on how to assemble your mask. I won’t list them here but if you Google “free face mask pattern” you will have hundreds to choose from.
The first design I tried did not fit at all well, it did not include a nose clip so gaped either side of my nose, and when I talked it rode down, almost exposing my nostrils. I had a play with a few different templates in an attempt to find one that fitted well and this is what I found:
- Include a nose clip, this could be made from any bendable metal but aluminium or plastic coated metals are preferred since it will be washed and you don’t want the metal to rust, twisty ties are recommended by several makers.
- I found the pleated designs offered enough length to wrap under your chin and not move around when you talk.
- Make sure it is wide enough, the outer edges of your mask should extend beyond the outer corners of your eyes but not reach your hairline.
- Elastic or adjustable straps will help to accommodate different head sizes.

Washability
Another important consideration is washability. Coronaviruses, are an enveloped virus (this means they have a lipid [fatty] outer layer) this layer breaks down when exposed to detergents (just like washing up liquid cleaning greasy dishes), without its lipid envelope the virus is inactivated. This is why hand-washing with soap and water is so effective. Washing your face mask with detergent will also destroy virus particles trapped within its fibres. Making your masks machine washable makes it easy to ensure you never need to reuse a dirty mask, you just pop them in the machine with the rest of your washing.
I make my masks from machine washable materials. If you want to use paper towel or coffee filter papers in your mask, I would choose one of the mask designs with a filter pocket.
Are some materials toxic?
Yes, you do need to be careful, especially with HEPA filters, some of which contain fibreglass, you really don’t want to be inhaling microscopic fragments of that!
I also strongly recommend machine washing any fabrics you plan to use, partly because they sometimes shrink the first time they are washed but mainly to remove any size and other treatments left on the cloth during manufacturing.
Using masks while caring for someone with Covid-19 symptoms
I am surprised by how little this is discussed in the press, while various governments request or instruct us to wear masks when in potentially crowded public spaces and that healthcare professionals should were them as PPE when treating patients there is rarely any mention of using them in the home if you are isolating with someone with Covid-19 symptoms.
Wherever possible, the sick person should isolate themselves in one room as much as possible, if they need to leave that room (to got to the bathroom for example) I recommend they should wear a mask. Similarly, if anyone needs to enter their room, I think it is a wise precaution for both parties to wear a mask, the only exception is if the sick person is struggling to breathe, in which case you probably should be calling for an ambulance.
In summary
- Homemade face masks worn in public spaces, where social distancing is difficult, will help limit the spread of coronavirus but they are no replacement for good hand hygiene and social distancing.
- Include a nose clip in your masks to achieve a good fit.
- The best materials for constructing your masks include, quilter’s cotton, polyester chiffon, flannel and natural silk. Layering a combination of different materials in the same mask is likely to produce the best filtration and may be on a par with N95 masks.
- At least 2 layers of fabric is advisable but be wary of using too many layers, you still need to be able breath through your mask (not around it!)
- Always wash and dry your mask after each use.
- Please leave the medical grade masks for the medics and give yourself a pat on the back for not only helping them but investing in a reusable face mask that is better for the environment too 🙂
If you would prefer to buy a ready-made reusable mask rather than make your own please take a look… https://www.etsy.com/uk/shop/TeriBerryTextiles?ref=seller-platform-mcnav§ion_id=28613742
Stay safe
References
Abhiteja Konda, Abhinav Prakash, Gregory A. Moss, Michael Schmoldt, Gregory D. Grant, Supratik Guha. Aerosol Filtration Efficiency of Common Fabrics Used in Respiratory Cloth Masks. ACS Nano, 2020
Mizumoto K and Chowell G. Transmission potential of the novel coronavirus (COVID-19) onboard the diamond Princess Cruises Ship 2020. Infectious Disease Modelling 2020. 5: 264-270
Nishiura H et al. Estimation of the asymptomatic ratio of novel coronavirus infections (COVID-19). Int J Infect Dis doi: 10.1016/j.ijid.2020.03.020
van der Sande – Professional and Home-Made Face Masks Reduce Exposure to Respiratory Infections among the General Population, 2008
Zayas G et al. Cough aerosol in healthy participants: fundamental knowledge to optimize droplet-spread infectious respiratory disease management. BMC Pulmonary Medicine 2012, 12:11
